Background information
Radiation therapy is a common cancer treatment that uses high-energy x-rays to kill cancer cells or sto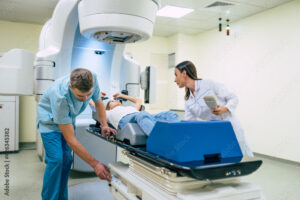 p them from growing and dividing. It’s a localized treatment, meaning it targets specific areas of the body where cancer cells are present while minimizing damage to healthy surrounding tissue. The treatments are individually designed for each person’s anatomy and treatment target area; thus precision is required to deliver the planned dose. There are many factors that contribute to differences between the planned dose and the delivered dose. One such factor is reproducibility in patient position on the treatment unit. Patient positioning is crucial in radiation therapy because it ensures accurate delivery of radiation to the targeted area while minimizing exposure to surrounding healthy tissues.
p them from growing and dividing. It’s a localized treatment, meaning it targets specific areas of the body where cancer cells are present while minimizing damage to healthy surrounding tissue. The treatments are individually designed for each person’s anatomy and treatment target area; thus precision is required to deliver the planned dose. There are many factors that contribute to differences between the planned dose and the delivered dose. One such factor is reproducibility in patient position on the treatment unit. Patient positioning is crucial in radiation therapy because it ensures accurate delivery of radiation to the targeted area while minimizing exposure to surrounding healthy tissues.
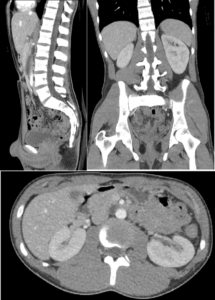
To ensure accurate patient positioning, image matching happens prior to each treatment and is performed while the patient is laying on the treatment couch waiting for the radiation beam to start. This is called Image Guided Radiation Therapy, or IGRT. Image matching in short, is looking at the image from the original “planned” treatment and matching it to the daily image of the patient on the treatment couch, the discrepancies are noted, bed movements are entered into the software which results in the patient moving to a position that matches the planned treatment image. Cross-sectional anatomy is included in the foundation of successfulimage matching. Acquiring and improving this skill is important to the success of the patient’s treatment as it is imperative that image matching is done in a time sensitive manner, to avoid any further patient movements. This course presents the function and application of Computed Tomography (CT) in the context of IGRT. The overarching goal is to provide students with a solid understanding of cross-sectional anatomy and its significance as it applies to IGRT.
laying on the treatment couch waiting for the radiation beam to start. This is called Image Guided Radiation Therapy, or IGRT. Image matching in short, is looking at the image from the original “planned” treatment and matching it to the daily image of the patient on the treatment couch, the discrepancies are noted, bed movements are entered into the software which results in the patient moving to a position that matches the planned treatment image. Cross-sectional anatomy is included in the foundation of successfulimage matching. Acquiring and improving this skill is important to the success of the patient’s treatment as it is imperative that image matching is done in a time sensitive manner, to avoid any further patient movements. This course presents the function and application of Computed Tomography (CT) in the context of IGRT. The overarching goal is to provide students with a solid understanding of cross-sectional anatomy and its significance as it applies to IGRT.
The target audience for this course is adult learners who have chosen to work in health care. They have a minimum of two years undergraduate prerequisite courses as well as so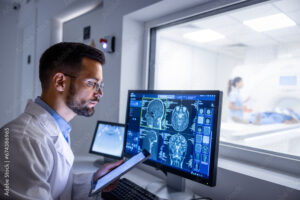 me radiation therapy course prerequisites. Information in these pre-requisite courses include how CTscanners and Linear Accelerators work, 2D- radiographic anatomy and how knowledge of the lymphatic system is applied in radiation therapy.
me radiation therapy course prerequisites. Information in these pre-requisite courses include how CTscanners and Linear Accelerators work, 2D- radiographic anatomy and how knowledge of the lymphatic system is applied in radiation therapy.
The learners in this type of program are usually young adults with a wide variety of lived experiences. Academically speaking, some come directly from completing the required 2 years of undergrad courses, and others with a variety of type and number of degrees. In other ways, some have not yet left the family home, some have children, some have done extensive travelling, some are changing careers. Some have worked in hospitals; some have never been inside a hospital.
Design
This course is a blended design scheduled in weekly modules. It follows a flipped classroom model, as the benefits of this strategy align with this topic. The course includes asynchronous didactic material, weekly discussion boards and one synchronous online class meeting. Every other week there is a face-to-face lab session scheduled for hands on learning and skill practice. The tools used to deliver this course and their application are as follows:
Canvas provides the learning management system (LMS) to host content such as didactic modules that may contain documents, videos, quizzes, discussion forums, collaborations, and student progress/grades.
Zoom provides the platform for the weekly synchronous class meetings. Screen sharing and the whiteboard are key functions for this activity.
ARIA software suite provides the image matching software for hands-on practice. This is only accessible within the CancerCare system.
IMAIOS provides high-quality cross-sectional anatomy and imaging content for daily practice and training of health professionals. This software offers a choice of regular, practice or quiz viewing mode to the learners.
The specific course objectives are listed here.
By the end of this course, learners will be able to:
- List and explain the three cardinal viewing planes of CT imaging.
- Using directional terms, describe the position of one anatomical structure as it relates to the position of another.
- Explain the orientation of a CT cross-sectional image.
- Compare the location of various structures between a cross sectional image and radiographic anatomy.
- Describe the boundaries of and the anatomic structures contained within the: thorax, abdomen, and pelvis
- Complete image matching on a variety of anatomical sites.
- Explain how the Choose Wisely and Image Gently campaigns apply to Image Guided Radiation Therapy.
These learning objectives are met by providing didactic course modules for learning and virtual tools for practicing cross-sectional anatomy identification and image matching. To see the course layout in more detail, view the course ADDIE Template here. The formative and summative assessments of learning address the three learning domains, Cognitive, Psychomotor and Affective.
Formative assessment opportunities include assignments, multiple choice review questions/polls, discussions and exit slips during synchronous class meeting, discussion boards, module quizzes, and clinical reviews.
Two Summative assessment strategies are used. A final exam and a final clinical assessment where the students are required to complete an Image Matching task.
Risk Assessment
Any online delivery is susceptible to certain risks and barriers. Addressing these risks and barriers requires proactive strategies and support from both educators and institutions.
Mitigation strategies need to address risks and barriers around technical issues, mental health, academic integrity and motivation.
Technical issue strategies involve providing access to technology and resources. The University of Winnipeg as well as the School of Radiation Therapy both provide resources such as space and technology to students who: do not have access to necessary devices such as a computer or tablet, struggle with reliable internet access, or struggle with finding appropriate spaces within their home for working.
Mental health strategies include surveying students about how they feel regarding online learning. This is followed by addressing any concerns that are self-perceived or suspected by the instructor, according to school policies. Online learning can be an isolating environment that leads to disconnection between students and/or instructor. The bi-weekly face-to-face Clinical Development Activities should help mitigate any concerns.
Maintaining academic integrity risk strategies recognize that online assessments can be vulnerable to cheating and plagiarism. Online quizzes do use such strategies as randomizing not only the quiz questions, but the order of the multiple-choice answers. In addition, the lock down browser can be used at the instructor’s discretion. However, relying on individual integrity has been the approach of the School of Radiation Therapy. Guiding the students to understand the links between academic integrity and their future as ethical professionals can mitigate integrity breaches. This strategic approach involves communicating this message early and throughout their training.
Online learning has shown to affect a learner’s motivation. However, most adult learners are intrinsically motivated to succeed. In this case, their goal is to become the professional that they have chosen as their career.
“Adults are motivated to learn to the extent that they perceive that learning will help them perform tasks or deal with problems that they confront in their life situations. Furthermore, they learn new knowledge, understandings, skills, values and attitudes most effectively when they are presented in the context of application to real-life situations.”
However, these young adult learners may still have under-developed self-discipline and time management skills. Therefore, a small amount of the final grade is given towards class participation.
If a learner requires extra time to gain the required proficiency prior to clinical placement, this will be arranged on a as needed basis.
Course design and rationale
I believe that no professional healthcare program can be taught exclusively online; nor does it have to be taught exclusively face-to-face. My assertion comes from two variables: the type of work they are learning to do and the uniqueness of the adult learner. The hybrid model is a great way to meet the needs of this group of adult learners; which is important to reaching my goal of developing empathetic, competent healthcare workers.
This course is designed within a hybrid learning environment. Rationale for each approach is described below.
Asynchronous Didactic Learning – Adult learning is less abstract and more goal oriented. They are more autonomous. They are responsible for their learning, which means being prepared for synchronous sessions, especially in a flipped classroom model. They have a full life outside of the program. These learners have family obligations, work obligations and hopefully a social life to keep them balanced. Time management is key to success in this group.
As image matching is completed on computers using special software, this approach to learning is ideal. The students will see the images
Synchronous Class Meetings – Adult learners are ready to learn, which can help with engagement, and their lived experiences can lead to deeper, more meaningful class discussions. Although I have experienced that this is very dependent on the group dynamic. Some classes are quite dynamic and others are not.
Face-to-Face Clinical Development Activities – Adult learners do well with practical applications where the didactic knowledge can be applied and transferred to practice. This course leverages this fact as it is necessary for labs to happen prior to any clinical placement so the learners can practice using the matching software (this cannot be done online as this software cannot be accessed outside of the institution). Here they will practice the specific task that will be required of them when they enter the clinical environment. Initially, the focusin on accuracy. Subsequently, the students’ goal is to to increase their skills to complete the task more quickly by the end of the semester.
While facilitating these sessions, the facilitators can vocalize their decision process, role modelling the importance of each step with the patients’ outcome in mind. As well, simulating the interaction between caregiver and patient, the instructors can role model the care and attention given to psychosocial needs within a certain clinical environment or situation.
Patients need to be the centre of all that is taught and learned. Not only does patient care need to be comprehensive, and delivered by skilled staff, it also must address the psychosocial needs of the patients. Empathy and compassion also contribute to patient outcomes. Online environments cannot transfer these lessons adequately. Of course, instructors provide real life examples that can convey the messages, but it is the real-life clinical environment where this learning occurs. In addition to the formal learning, there exists a hidden curriculum that cannot be ignored. Hidden curriculum can be explained as how unwritten rules are transmitted to the learners. A few examples are workplace cultures, norms, authority structures, gender roles, implicit biases, and attitudes. Over the years the term ‘hidden curriculum’ has been used to describe how negative behaviours, stereotypes, and biases are passed along within the profession. However, it is important to be aware of the hidden curriculum and teach positive lessons through everyday interactions while the learner is still developing their own perception of what it means to them to work as such a PHC provider. This is the instructor’s opportunity to teach honesty, transparency, and integrity to the learners through role modelling.
All three learning domains will be addressed as each plays their own role and are important in this task and career.
The cognitive domain is addressed within the didactic portion of this course through lessons, assignments and quizzes. These should be completed by the learners by the time the synchronous activities are scheduled.
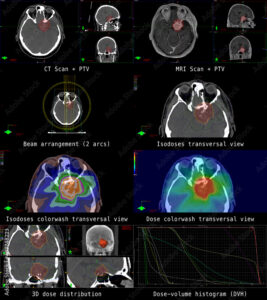
Clinical Development Activities, or labs, cover the psychomotor domain. Students will be scheduled in small groups on the RT machines, either on weekends or after hours (as operational requirements permit). Here they will practice the specific task that will be required of them when they enter the clinical environment. Initially, the focus in on accuracy. Subsequently, the students’ goal to increase their skills to complete the task more quickly by the end of the semester. Some learners may require more time to gain the required proficiency than can be provided due to limitations in the availability of both clinical space and staff facilitators.
Discussion groups and clinical development activities will cover the Affective domain. Students will demonstrate the patient centred approach to IGRT through discussion and they will learn from their clinical role models in the Clinical Development Activities.





 I am using the LMS
I am using the LMS  p them from growing and dividing. It’s a localized treatment, meaning it targets specific areas of the body where cancer cells are present while minimizing damage to healthy surrounding tissue. The treatments are individually designed for each person’s anatomy and treatment target area; thus precision is required to deliver the planned dose. There are many factors that contribute to differences between the planned dose and the delivered dose. One such factor is reproducibility in
p them from growing and dividing. It’s a localized treatment, meaning it targets specific areas of the body where cancer cells are present while minimizing damage to healthy surrounding tissue. The treatments are individually designed for each person’s anatomy and treatment target area; thus precision is required to deliver the planned dose. There are many factors that contribute to differences between the planned dose and the delivered dose. One such factor is reproducibility in  laying on the treatment couch waiting for the radiation beam to start. This is called Image Guided Radiation Therapy, or IGRT.
laying on the treatment couch waiting for the radiation beam to start. This is called Image Guided Radiation Therapy, or IGRT.  me radiation therapy course prerequisites. Information in these pre-requisite courses include how CTscanners and
me radiation therapy course prerequisites. Information in these pre-requisite courses include how CTscanners and 


 Before I start this course, I wanted to spend a few minutes reflecting on what digital technology meant and how it is changing. Prior to 2020, digital content in my classroom meant saving larger files on the shared drive to save paper. It meant delivering the class content via PowerPoint and demonstrating examples on the white board. This picture is not my classroom, but it is surprisingly similar. Just like the instructor of this classroom, I had a tiny space of white board available behind the podium to the left of the screen to do physics equations, draw pictures of diverging radiation beams and stick figure patients. Utilizing more whiteboard space meant rolling up the screen, then pulling it down to continue with the slides – covering up the example I just drew on the board!
Before I start this course, I wanted to spend a few minutes reflecting on what digital technology meant and how it is changing. Prior to 2020, digital content in my classroom meant saving larger files on the shared drive to save paper. It meant delivering the class content via PowerPoint and demonstrating examples on the white board. This picture is not my classroom, but it is surprisingly similar. Just like the instructor of this classroom, I had a tiny space of white board available behind the podium to the left of the screen to do physics equations, draw pictures of diverging radiation beams and stick figure patients. Utilizing more whiteboard space meant rolling up the screen, then pulling it down to continue with the slides – covering up the example I just drew on the board! Another piece of technology I incorporated into my lessons was the iClicker. There are newer tools to engage students, but it worked well, and allowed me to assess the level of knowledge transfer. The pandemic forced us all to learn quickly and change our teaching methods to deliver the same content over an online platform, Zoom in my case. How do we deliver quizzes? How do we uphold the integrity of the test material? Eventually solutions to these challenges emerged.
Another piece of technology I incorporated into my lessons was the iClicker. There are newer tools to engage students, but it worked well, and allowed me to assess the level of knowledge transfer. The pandemic forced us all to learn quickly and change our teaching methods to deliver the same content over an online platform, Zoom in my case. How do we deliver quizzes? How do we uphold the integrity of the test material? Eventually solutions to these challenges emerged.